Connect With Us
Blog
Clubfoot and Early Care for Healthy Development

Clubfoot is a congenital foot deformity in which the foot is twisted inward and the toes point downward. It may affect one or both feet and is present at birth. This condition is often linked to genetic factors and differences in muscle and tendon development. Symptoms include a visible inward position of the foot, limited range of motion, and stiffness in the affected area. Early care is important to support proper alignment and function as a child grows. A podiatrist can assess the condition, guide treatment options, and monitor progress to improve mobility and comfort. With timely care, many children achieve strong and functional movement. If your child has been born with symptoms of clubfoot, it is strongly suggested that you promptly schedule a visit with a podiatrist to support healthy foot development.
Congenital foot problems require immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of Footcare Now. Our doctors can provide the care you need to keep you pain-free and on your feet.
Congenital foot problems are deformities affecting the feet, toes, and/or ankles that children are born with. Some of these conditions have a genetic cause while others just happen. Some specific foot ailments that children may be born with include clubfeet, polydactyly/macrodactyly, and cleft foot. There are several other foot anomalies that can occur congenitally. What all of these conditions have in common is that a child may experience difficulty walking or performing everyday activities, as well as trouble finding footwear that fits their foot deformity. Some of these conditions are more serious than others. Consulting with a podiatrist as early as possible will help in properly diagnosing a child’s foot condition while getting the necessary treatment underway.
What are Causes of Congenital Foot Problem?
A congenital foot problem is one that happens to a child at birth. These conditions can be caused by a genetic predisposition, developmental or positional abnormalities during gestation, or with no known cause.
What are Symptoms of Congenital Foot Problems?
Symptoms vary by the congenital condition. Symptoms may consist of the following:
- Clubfoot, where tendons are shortened, bones are shaped differently, and the Achilles tendon is tight, causing the foot to point in and down. It is also possible for the soles of the feet to face each other.
- Polydactyly, which usually consists of a nubbin or small lump of tissue without a bone, a toe that is partially formed but has no joints, or an extra toe.
- Vertical talus, where the talus bone forms in the wrong position causing other bones in the foot to line up improperly, the front of the foot to point up, and the bottom of the foot to stiffen, with no arch, and to curve out.
- Tarsal coalition, when there is an abnormal connection of two or more bones in the foot leading to severe, rigid flatfoot.
- Cleft foot, where there are missing toes, a V-shaped cleft, and other anatomical differences.
- Macrodactyly, when the toes are abnormally large due to overgrowth of the underlying bone or soft tissue.
Treatment and Prevention
While there is nothing one can do to prevent congenital foot problems, raising awareness and receiving neonatal screenings are important. Early detection by taking your child to a podiatrist leads to the best outcome possible.
If you have any questions, please feel free to contact our offices located in Elmhurst Jackson Heights, Astoria, Rego Park, and Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
When Foot Surgery May Be Necessary and What to Expect
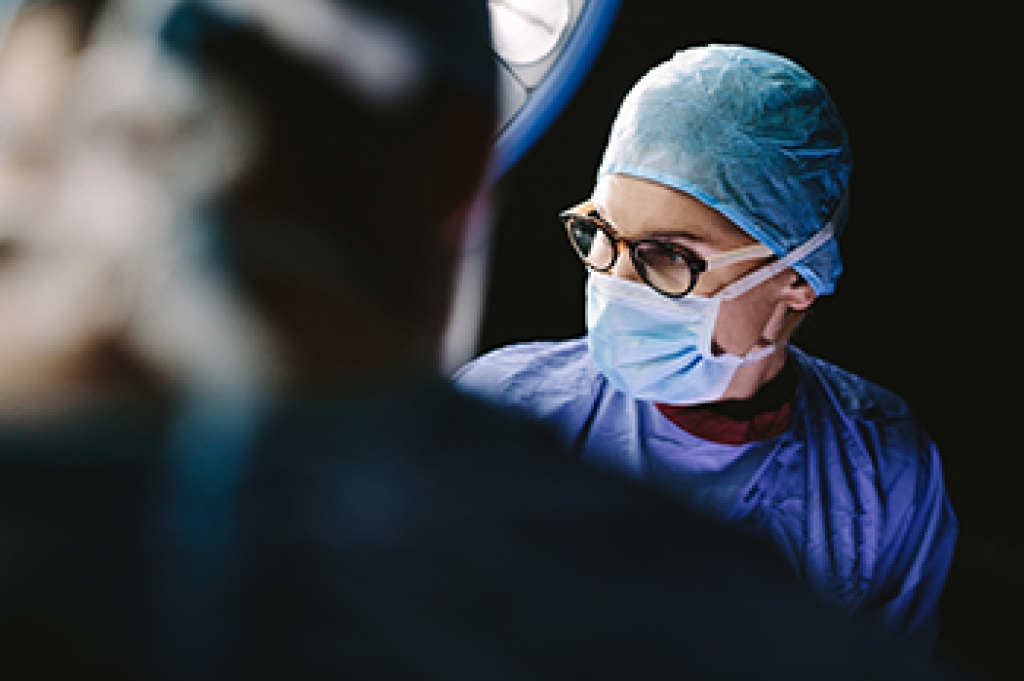
Foot surgery may be recommended when conservative treatments fail to relieve pain or restore function. Many conditions, such as bunions, hammertoes, plantar fasciitis, arthritis, or tendon injuries, are first treated with rest, orthotics, medications, or targeted exercises. When these measures do not provide adequate relief, surgical intervention may help correct deformities, reduce pain, and improve mobility. Procedures vary depending on the condition, and may involve realigning bones, repairing soft tissue, or fusing joints. While surgery can be effective, it is not without risks. Possible complications include infection, nerve irritation, prolonged swelling, stiffness, or delayed healing. Recovery time can also vary and may require limited weight-bearing and rehabilitation. Careful evaluation and discussion of options are important before proceeding. If you are experiencing persistent foot pain despite treatment, it is suggested that you see a podiatrist for an evaluation and guidance.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact one of our podiatrists of Footcare Now. Our doctors will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions, please feel free to contact our offices located in Elmhurst Jackson Heights, Astoria, Rego Park, and Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Finding Relief From Achilles Tendon Pain

Achilles tendinopathy is a condition involving irritation and breakdown of the Achilles tendon, the thick band that connects the calf muscles to the heel bone. Diagnosis begins with a careful exam, where a podiatrist checks for pain, swelling, and stiffness along the back of the heel, especially with movement or pressure. Imaging such as an ultrasound or MRI scans may be used to confirm changes in the tendon structure. Treatment focuses on reducing strain and supporting healing. This may include activity changes, wearing supportive shoes, heel lifts, and guided stretching and strengthening exercises. Targeted exercises can help improve tendon function, over time. In some cases, advanced options may be considered. Ignoring symptoms can lead to worsening damage. If heel pain is ongoing or limiting activity, it is suggested that you see a podiatrist for an evaluation, diagnosis, and appropriate care.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact one of our podiatrists of Footcare Now. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our offices located in Elmhurst Jackson Heights, Astoria, Rego Park, and Forest Hills, NY . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Diabetes and Protecting Your Feet
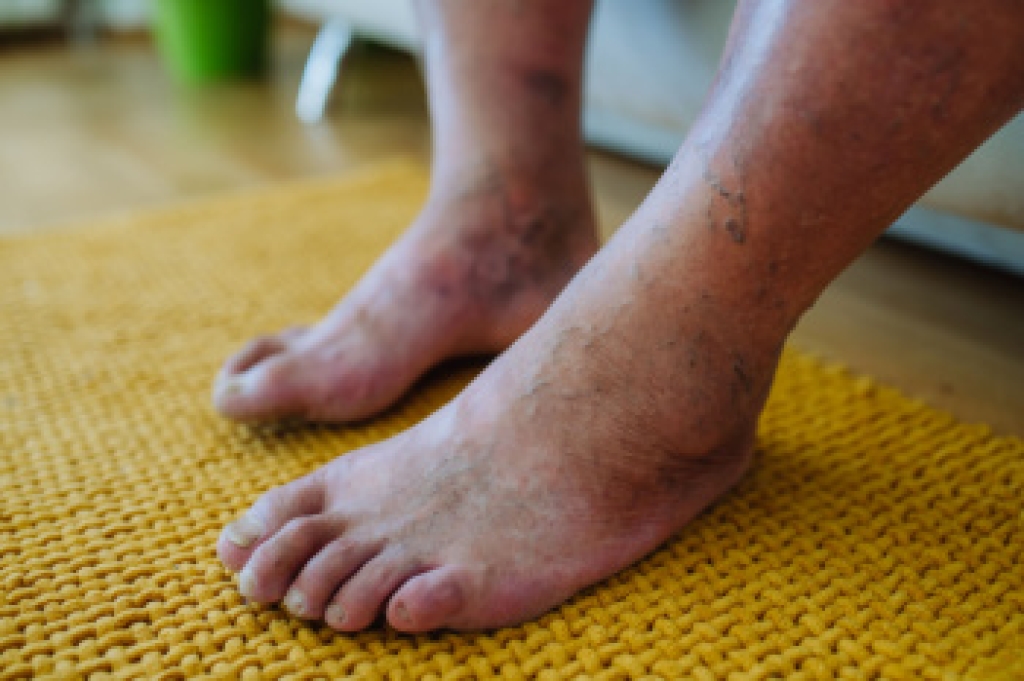
Diabetes can affect multiple systems in the body, including the eyes, nerves, and circulation, all of which play a role in foot health. Retinopathy damages the blood vessels in the eyes and can reduce vision, making it harder to notice cuts, sores, or changes in the feet. Neuropathy affects the nerves and may cause numbness or burning, so injuries can go unnoticed. Circulation problems can slow healing, increasing the risk of infection. Together, these issues can raise the chance of serious foot complications if not managed carefully. Regular monitoring is critical to catch problems early. A podiatrist is an important part of the health care team, providing routine exams, treating wounds, and helping prevent complications through proper foot care and footwear guidance. If you are managing diabetes and have foot concerns, it is suggested that you schedule routine appointments with a podiatrist.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact one of our podiatrists from Footcare Now. Our doctors can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions, please feel free to contact our offices located in Elmhurst Jackson Heights, Astoria, Rego Park, and Forest Hills, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blog Archives
- 2026
- 2025
- 2024
- 2023
- 2022
- 2021

